Practice of Axilla Surgery · 2016-09-28 · 1 T3, clinically positive axilla and biopsy- proven...
Transcript of Practice of Axilla Surgery · 2016-09-28 · 1 T3, clinically positive axilla and biopsy- proven...
Practice of Axilla Surgery
Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy
연세의대 외과
박세호
Summer School of Breast Disease 2016
Contents
• Anatomy of the axilla
• Axillary lymph node dissection (ALND)
• Sentinel lymph node biopsy (SLNB)
• ASCO guideline and updates
Borders of the axilla - like a pyramid -
• Apex (axillary inlet) : lateral border of the first rib, superior border of scapula, & posterior border of clavicle
• Lateral wall : intertubecular groove of humerus.
• Medial wall : serratus anterior & thoracic wall (ribs, intercostal m.)
• Anterior wall : pectoralis major, pectoralis minor, & subclavius m.
• Posterior wall : subscapularis, teres major, & latissimus dorsi
• Base : skin
Motor nerves
Winged scapula Shoulder apraxia
Impaired arm abduction
Atrophy and shortening of pectoral muscle
The Impact of ALND
Clearance of Regional Disease
Improve chance of cure
Survival benefit
Staging - Prognostic factor - Adjuvant therapy
Kim et al. J Breast Cancer 2014;17(2):99-106.
Indication for ALND • 감시림프절 생검술에서 전이를 보이는 경우
• 감시림프절 생검의 금기 또는 감시림프절을 찾지 못한 경우
• 염증성 유방암에서 선행화학요법 후 수술시
• 감시림프절 생검술 후 액와부 림프절 지역재발의 경우
감시림프절을 벗어난 액와부 림프절의 전이의 가능성이 높거나 확인된 경우.
Disease of the Breast 5th ed.
Indications for ALND in the Era of SLN Biopsy
Patients outside the ACOSOG Z0011 entry criteria1
Prior inadequate ALND
Validation trials of SLN biopsy
Failed SLN biopsy
Clinically suspicious nodes identified at surgery
T4 disease
Unavailability of SLN biopsy
Axillary local recurrence (ipsilateral or contralateral) in previously treated patients
1 T3, clinically positive axilla and biopsy-proven nodal metastasis, positive SLN with disease requiring mastectomy, more than 2 positive SLNs or matted axillary nodes.
Contraindication for ALND • 임상적으로 임파절 전이가 없을 때 감시림프절 생검술상 음성시
• Ductal carcinoma in situ / Lobular carcinoma in situ
액와부 림프절의 전이의 가능성이 낮거나 음성이 확인된 경우.
Preoperative preparation
• Axillary shaving
• Pad for arm board – Preventing shoulder dislocation – Preventing brachial plexus tension injury
• Broad spectrum antibiotics IV just before surgery
• Short term muscle relaxant
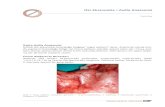
Procedures of ALND (I)
• Identification of landmark -> pectoralis muscles, LD • Opening of clavipectoral fascia • Preservation of axillary vein,
artery and brachial plexus • Preservation of medial / lateral
pectoral nerves • Ligation of braches of axillary
vein
Procedures of ALND (II) • Mobilization of axillary fat pad • Identification of intercostobrachial nerve • Identification of motor nerves (long thoracic nerve &
thoracodorsal neurovascular bundle)
Extents of ALND
• Level I & II : standard levels of dissection
• Interpectoral nodes (Rotter’s node) • Level III → only in cases with gross disease in level II • More than 10 nodes retrieved by pathologic
examinations
Complications of ALND
• Pain, axillary web syndrome • Hematoma or seroma • Infection • Lymphedema : ~30% • Shoulder dysfunction • Weakness or Numbness • Op time, Cost • Morbidity
Lymphatic drainage of breast
76~95%
1.3~9.9%
Sappey’s subareolar plexus (1874년) Ann Surg Oncol 2008;(3):863-871
Sentinel lymph node • The first LN in the chain of nodes that forms the regional
lymphatic system • A key indicator of axillary metastasis in breast cancer • Can be identified using radioactive colloids with or without
blue dye (lymphatic mapping) Radioactive colloid
• Entrapped within the SLN through – A function of their particular
size – Phagocytosis by leukocyte
• Between 2 and 24 h before surgery
• Localization of nano-colloid in the SLNs
Vital dye • Bind to interstitial albumin, and
taken up by local lymphatic tissue – Lymphatics are converted to
bright blue channel • Intraoperative injection • Directs to the lymphatics that
tract to the SLNs
Lymphatic mapping Radioisotope with lymphoscintigraphy
• Detected by gamma probe
10% rule • Removal of all SLNs with
counts over 10% of the most radioactive node (hot nodes)
Lymphatic mapping Vital blue dye
• Isosulfan blue – Albumin과 결합하여 선택적으로 림프관을 따라 이동
– 림프관 및 감시림프절을 파랗게 염색시킴.
• Methylene blue, Indigo carmine, patent blue V, Indigo cyanine green
Advantages of SLNB
• Compared to ALND,
• Less infection • Less lymphedema • Less shoulder dysfunction • Less weakness, pain • Not inferior accuracy for staging
ASCO guideline updates in 2014 • 권고안 1. 조기 유방암 환자에서 감시림프절 전이가 없을 경우 액와림프절 곽청술을 권고해서는 안
된다.
• 권고안 2.1 유방보존술 후 전유방 방사선 치료가 예정되어 있으면서, 1~2개의 감시림프절 전이가 발견된 조기 유방암 환자의 경우 액와림프절 곽청술을 권고해서는 안 된다.
• 권고안 2.2 유방전절제술이 계획된 조기 유방암 환자에서 감시림프절 전이가 발견된 경우 액와림프절 곽청술을 제안해도 된다.
• 권고안 3. 아래와 같은 상황에 있는 수술이 가능한 유방암 환자의 경우 감시림프절 생검술을 제안해도 된다.
– 3.1 Multicentric tumors – 3.2 유방전절제술이 필요한 상피내암 – 3.3 이전에 유방이나 액와부에 수술을 시행했던 경우 – 3.4 수술전 항암화학요법을 시행한 경우
• 권고안 4. 아래와 같은 상황에 있는 조기 유방암 환자에서 감시림프절을 시행해서는 안 된다고 규정한 2005년도 권고안을 바꿀만한 충분한 근거는 아직 없다.
– 4.1 종양이 크거나 국소진행성 유방암의 경우 (Tumor size T3/T4) – 4.2 염증성 유방암 – 4.3 유방보존술이 예정된 상피내암 – 4.4 임신의 경우
ACOSOG Z0011
Primary Objective -> To assess whether OS after SLND alone was not inferior to that for patients who underwent completion ALND for a positive SLN
Z0011 eligibility
Eligible
• Clinical T1-2N0 breast cancer
• H&E-detected SLN metastases
• Lumpectomy + Whole breast RT
• Adjuvant systemic Tx by choice
Ineligible
• Nodal RT • IHC-detected SLN
metastases • Matted nodes • 3 or more involved SN
Giuliano AE et.al. Ann Surg 2010;252:439
Z0011 locoregional recurrence
Giuliano AE et.al. Ann Surg 2010;252:439
Additional positive nodes in 27% of ALND’s
Recurrence SLN+ ALND
(n=388)
SLN+ no ALND (n=425)
local 3.6% 1.9%
regional node 0.5% 0.9%
local+regional 4.1% 2.8%
P = 0.47