PANKREATITIS IPD
-
Upload
yonathanhasudungan -
Category
Documents
-
view
251 -
download
10
description
Transcript of PANKREATITIS IPD

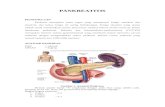
Pankreatitis

Pancreatitis
Definition and Etiology
An inflammation process of the pancreas with associated escape of the pancreatic enzyme into surrounding tissue.
The primary etiologic factors are alcoholism & biliary tract disease.
May be a complication of viral or bacterial disease, peptic ulcer, trauma.

Pancreatitis
Incidence & Risk Factors
Major- Biliary stones, Alcohol use/abuseMinor- Age: 55 to 65 yrs. for biliary
pancreatitis 45- 55 yrs. For alcohol-related Female for biliary tract pancreatitis; Male-
for alcohol-related pancreatitis.Trauma, Infectious disease, drug toxicities,
chronic diseases( inflammatory diseases).

Table 1. Causes of acute pancreatitis
AlcoholAutoimmuneBiliary (eg, gallstones, gallbladder microlithiasis/sludge)Drug-induced (see Table 2)Iatrogenic
Surgery (eg, common bile duct exploration, sphincterotomy, splenectomy, distal gastrectomy)ERCP
IdiopathicInfectious (eg, ascariasis, clonorchiasis, mumps, toxoplasmosis, coxsackievirus, cytomegalovirus, tuberculosis, Mycobacterium avium complex)Inherited
CFTR (cystic fibrosis transmembrane conductance regulator) mutationsSPINK1 (serine protease inhinitor Kazal type 1) mutationsPRSS1 (cationic trypsinogen) mutations
Metabolic (eg, hypercalcemia, hypertriglyceridemia)Neoplastic (eg, pancreatic or ampullary tumors)Structural (eg, pancreatic divisum, annular pancreas, sphincter of Oddi dysfunction, periampullary diverticula, duodenal duplication cysts, choledochocele, anomalous pancreaticobiliary junction, regional enteritis)Toxic (eg, organophosphates, scorpion venum)Traumatic (especially motor vehicle accidents)Vascular
- in USA, gallstone & alcohol abuse

Table 2.Drugs implicated in acute pancreatitis based on class
Class IAa Class IBb Class IIcα-Methyldopa All-transretinoic acid AcetaminophenArabinoside Amiodarone ChlorothiazideAzodisalicylate Azathioprine ClozapineBezafibrate Clomiphene Dideoxyinosine (DDI)Cannabis Dexamethasone ErythromycinCarbimazole Ifosfamide EstrogenCodeine Lamivudine L-AsparaginaseCytosine Losartan PegasparaginaseDapsone Lynesterol/methoxyethinylestradiolPropofolEnalapril 6-mercaptopurine TamoxifenFurosemide MeglumineIsoniazid MethimazoleMesalamine NelfinavirMetronidazole Norethindronate/mestranolPentamidine OmeprazolePravastatin PremarinProcainamide SulfamethoxazolePyritinol Trimethoprim-sulfamethoxazoleSimvastatinStibogluconateSulfamethoxazoleSulindacTetracyclineValproic acid

Pancreatitis Ranson’s criteria
Admission criteria Criteria during initial 48 hours
Age: 55 yrs. Or older Hct: decrease or more than 10%
WBC: 16,000/mm3 or higher
BUN:increase greater than 5 mg/dl.
LDH: 350 IU/L or higherGlucose > 200 mg/dl.
CA: falls to less than 8 mg/dl.PaO2 < 60 mm Hg
AST: 250 U/L or higher Fluid sequestration; greater than 6 liter.

Table 3. Causes of idiophatic or unexplained acute pancreatitis diagnosed by endoscopic evaluation.*
Ampullary lesionsCholedocholithiasisChronic pancreatitisGallbladder microlithiasis or sludgePancreas divisumPancreatic cancerSphincter of Oddi dysfunction
*Exclusion of hyperlipidemia and medications.

Pathogenesis
The latest discovery specifically for hereditary pancreatitis is the discovery of trypsinogen gene mutations: PRSS1 and SPINK1, which leads to impaired balance between proteases and inhibitors in pancreatic parenchyma, causing activation of pancreatic Zymogen with the result of "autodigestion and inflammation". In turn acinar cell damage and improvement of inflammatory cell mediators.

Alcohol metabolism and biliary pancreatitis
•The mechanism that is clear, is because alcohol pancreatitis and acute biliary pancreatitis.
•Alcohol metabolism is the process of oxidative and nonoksidatif. Primary oxidative process takes place in the liver, whereas nonoksidatif in the pancreas. Nonoksidatif process will increase the formation of "fatty acid esters ethanol" (FAEEs).
•Biliary pancreatitis caused by the passage of gall bladder stone through the cystic duct into the CBD. Pinched stone in the ampulla Vater will cause reflux of bile into the pancreatic duct or pancreatic duct obstruction exit.

Pancreatitis Assessment
Pain:Steady & severe in nature; located in
the epigastric or umbilical region; may radiate to the back. Worsened by lying supine; may be lessened by flexed knee, curved-back position.
VomitingVaries in severity, but is usually protracted, worsened by ingestion of food or fluid. Does not relieve the pain. Usually accompanied by nausea.

Pancreatitis Assessment
Fever:Rarely exceeds 39 C.
Abdominal Finding:Rigidity, tenderness, guarding, distended, decreased or absent peristalsis and paralytic ileus.Fatty stools-(steatorrhea)
Laboratory Finding:Elevation of white count- 20,000-50,000.Elevated serum lipase and amylase(5 to 40 times); glucose, bilirubin, alkaline phosphatase. Urine amylase elevated. Abnormal low serum CA, Na & Mg.-due to dehydration. Binding of Ca in areas of fat necrosis.

Cullen Sign (periumbilical ecchymoses)

Grey Turner’s sign (flank ecchymoses)

Studi Imaging
- CT scan
- USG
- MRCP (Magnetic Resonance Cholangiopancreatography)

Idiophatic PancreatitisNegative CT,
negative serology,including lipids and metabolic
panelMRCP, EUS (if
available)CBD stones,pancreatic divisum,
Choledochocele,chronic
pancreatitis with PD stone
Tumor Gallbladder stones/sludge
Autoimmune pancreatitis Normal
Endoscopic therapy Surgery Cholecystectom
yGallbladder in
situ
Gallbladder out
ERCP with sphincter of Oddi manometry,
sphincterotomy if manometry abnormal
Observation
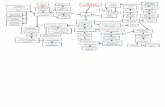
Algorithm for the evaluation & management of idiopathic pancreatitis. CBD: Common Bile DuctCT : Computed TomographyERCP : Endoscopic Retrogade CholangiopancreatographyEUS : Endoscopic UlatrasoundMRCP : Magnetic Resonance CholangiopancreatographyPD : Pancreatic Duct

Table 4. Differential diagnosis of acute pancreatitis.Perforated viscusCholecystitisBowel obstructionVascular occlusion (especially mesentery venous disease)Renal colicInferior myocardial infarctionPneumoniaDiabetic ketoacidosisDuodenal ulcer

Complication
1. Pancreatic Pseudocyst → Th/ Drainage
2. Abscess formation → Th/ Surgical drainage
3. Pancreatic ascites ∞ from pancreas duct disruption
4. Esophagogastric varices ∞ obstruction of vena lienalis pseudoaneurysm ∞> pseudocyst /
pancreatic necrosis5. Pancreatic Encephalopathy Subcutaneus Fat Necrosis Subcapsular Hematom LimpaRare

TherapyA.Mild Acute Pancreatitis
Supportive care • Bowel rest• IV Crystalloid• Analgesia
Pain –Nausea/vomiting –Bising usus +Analgesia –Hungry
Oral intake :Full liquid diet ↓Lowfat solid diet
Gallstone Pancreatitis : Lap-chole orEndoscopic biliarySphincterotomy

B. Severe Acute Pancreatitis
Fluid Resuscitation – check Ht every 12 hrsOrgan Failure – ICU
Nasojejunal Tube
Necrotizing Pancreatitis – enzym pankreas PPI AB Surgical debridement / Necrosectomy (3-
4week after medical therapy).
Urgent ERCP (in 24 hrs) for severe acute biliary pancreatitis.

Prognostic
Ranson criteriaOn admission
Age > 55 yearsWBC > 16.000/mm3Glucose > 200 mg/dlLactic dehydrogenase > 350 u/lAspartate aminotransferase (SGOT) > 250 u/l
After 48 hours of hospitalizationFall of hematocrit > 10 pointsIncrease of blood urea nitrogen > 2mg/dlSerum calcium < 8mg/dlArterial p O2 < 60 mmHgBase deficit > 5mEq/lFluid sequestration > 6 l

Chronic Pankreatitis

Table 5. TIGAR-O classification of chronic pancreatitis.
Toxic-MetabolicAlcoholicTobacco smokingHypercalcemia (hyperparathyroidism)Hyperlipidemia (rare and controversial)Chronic renal failure
IdiopathicCause unknown, likely genetic originTropical
GeneticAutosomal dominantCationic trypsinogenAutosomal recessive/modifier genesCFTR mutationsSPINK1 mutationsα₁-Antitrypsin deficiency (possible)
AutoimmuneIsolated autoimmune chronic pancreatitiAssociated with:
• Primary sclerosing cholangitis• Sjögren syndrome• Primary biliary cirrhosis• Type 1 diabetes mellitus
Recurrent and Severe Acute PancreatitisPostnecrotic (severe acute pancreatitis)Vascular diseases/ischemiaPostradiation exposure
ObstructionPancreas divisum (controversial)Sphincter of Oddy dysfunction (controversial)Duct obstruction (tumors, post-traumatic)

PathogenesisMorphological changes in chronic pancreatitis occurred in
ductus
Parenchym pankreas
• Dilated• Irregular• Strictured
Glandular tissue→ irregular & patchy→ fibrosis acinar cell
Hypothesis :1. The role of oxidative stress2. Toxic – metabolic causes3. Obstructive causes4. Necrosis – fibrosis (SAPE theory – Sentinel
Acute Pancreatitis Episode)

Gambaran Klinis
a. Sign and symptom50% case → * abdominal pain
* pancreatic insufficiency

b. Laboratorium1. Amylase & Lipase ↑↑2. Marker of pancreatic exocrine function is fecal pancreatic elastase-1 (FPE1). Normal: 200 mcg / g of faeces: severe exocrine.pancreatic insufficiency.3. HbA1c4. Marker Autoimmune : IgG4, RhF, ANA
c. Studi Imaging1. BNO 2. USG abdomen3. CT4. MRCP Magnetic Resonance Cholangiopancreatography5. EUS Endoscopic Ulatrasound6. ERCP Endoscopic Retrogade Cholangiopancreatography

Diagnosis Differential
Komplikasi
1. Peptic Ulcer2. IBD3. Gastric dysmotility4. IBS
1. Pseudocyst2. Billiary duct obstruction 3. Pancreatic ascites4. Pleural Effesion5. Thrombosis vena lienalis6. Pancreatic Fiastulae7. Pseudoaneurysm8. Risk↑ ca. pancreas

Proven Benefit Uncertain Benefit
Smoking cessationAlcohol cessationCoticosteroids for autoimmune pancreatitisAnalgesics
Pancreatic enzyme supplementationTranscranial magnetic brain stimulation
Table 6.Treatment options for chronic pancreatitis
If obstuction : invasive Th/* endoscopic clearance* surgical therapy* ESWL
-Pancreatico jejunostomy-Whipple procedure-Total pancreatectomy

References
1. Gastroenterology and . Ed. Gabriele Bianchi Porro. Mc. Graw Hill, 1999 pp. 205 – 233
2. Gastrointestinal System. Second Edition. Ed. Melanie Sarah Long. Mocby, 2002 pp. 103 – 113
3. Gastroenterology, Hepatology & Endoscopy. Ed. Norton J. Greenberger. Matt Large, 2009 pp. 291-309